A Patient’s Guide to Thumb Fusion Surgery
Introduction
Thumb arthritis may be surgically treated with a fusion procedure. The bones that form the thumb joint are set so they can grow together, or fuse. After fusing, the joint won’t move, and your pain should go away.
This guide will help you understand
- which parts of the thumb are involved
- why this type of surgery is used
- what happens during surgery
- what to expect before and after surgery
Anatomy
Which parts of the thumb are involved?
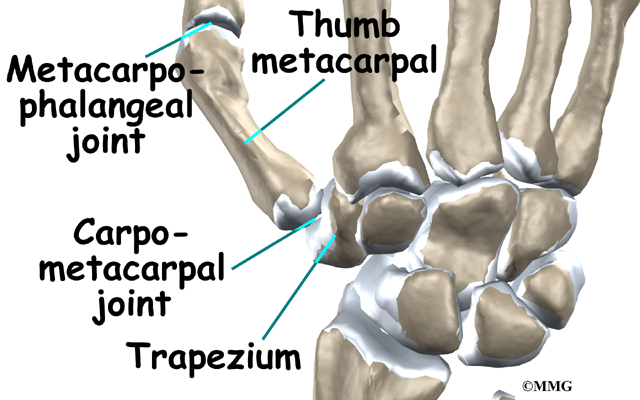
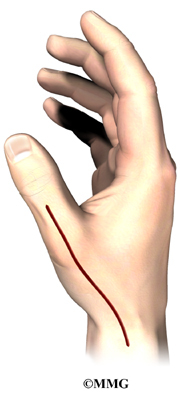
The CMC joint (an abbreviation for carpometacarpal joint) of the thumb is where the metacarpal bone of the thumb attaches to the trapezium bone of the wrist. This joint is sometimes referred to as the basal joint of the thumb. The CMC is the joint that allows you to move your thumb into your palm, a motion called opposition.
Several ligaments (bands of strong tissue) hold the joint together. These ligaments join to form the joint capsule of the CMC joint. The joint capsule is a watertight sac around the joint.
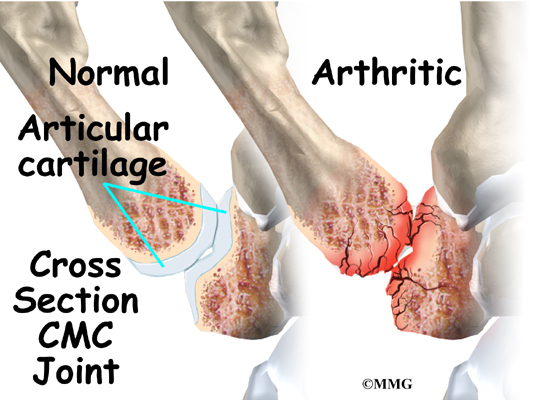
The joint surfaces are covered with a material called articular cartilage. This material is the slick, spongy covering that allows one side of a joint to slide against the other joint surface easily. When this material wears out, the joint develops a type of arthritis called osteoarthritis and becomes painful.
Related Document: A Patient’s Guide to Hand Anatomy
Rationale
What does the surgeon hope to achieve?
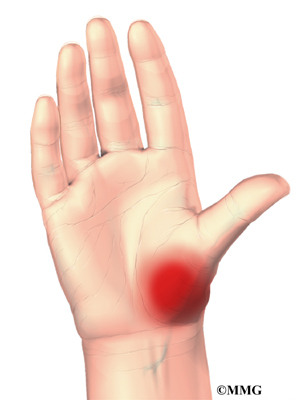
When the articular cartilage wears out, the CMC joint becomes arthritic. The joint becomes painful when the thumb is used for gripping and pinching.
Related Document: A Patient’s Guide to Arthritis of the Thumb
Joint fusion is a procedure that joins the surfaces of the thumb metacarpal and the trapezium so they don’t move or cause pain. This surgery is usually done on younger patients who have to have a lot of thumb strength on the job, such as carpenters who need to use a hammer all day. Once the CMC joint is fused, their pain goes away. They lose joint movement, but they still have a good ability to grip and pinch.
Preparations
What should I do to prepare for surgery?
The decision to proceed with surgery must be made jointly by you and your surgeon. You need to understand as much about the procedure as possible. If you have concerns or questions, you should talk to your surgeon.
Once you decide on surgery, you need to take several steps. Your surgeon may suggest a complete physical examination by your regular doctor. This exam helps ensure that you are in the best possible condition to undergo the operation.
On the day of your surgery, you will probably be admitted to the hospital early in the morning. You shouldn’t eat or drink anything after midnight the night before.
Surgical Procedure
What happens during the operation?
Surgery can last up to 90 minutes. Surgery may be done using a general anesthetic, which puts you completely to sleep, or a local anesthetic, which numbs only the hand. With a local anesthetic you may be awake during the surgery, but you won’t be able to see the surgery.
Once you have anesthesia, your surgeon will make sure the skin of your hand is free of infection by cleaning the skin with a germ-killing solution. An incision is made on the side of the thumb just over the CMC joint. Special care is taken not to damage the nearby nerves going to the thumb.
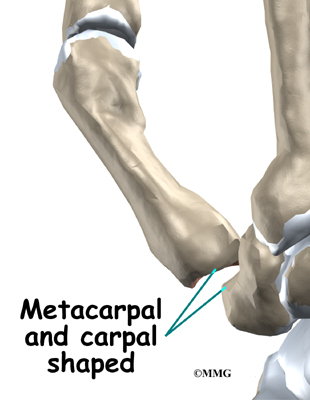
The joint capsule surrounding the CMC joint is then opened so that the surgeon can see the joint surfaces. The articular cartilage is removed from both joint surfaces to leave two surfaces of raw bone. A special tool is used to hollow the end of the thumb metacarpal to form a socket. The surface of the trapezium is shaped into a rounded cone that fits into the socket inside the thumb metacarpal.
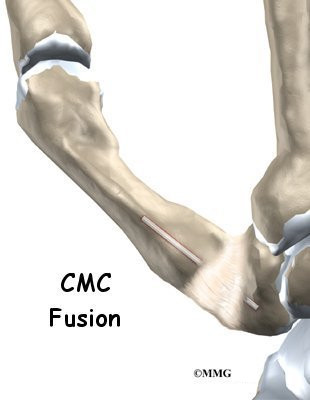
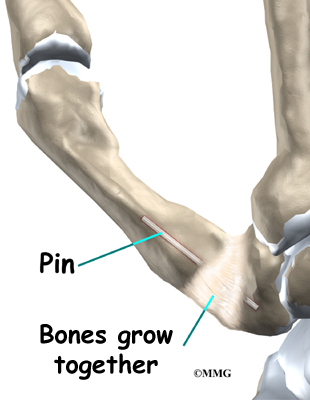
The surgeon places a metal pin through the center of both bones and then connects the cone and socket snugly together. A metal pin allows the surgeon to hold the two bones in the correct alignment and prevents the bones from moving too much as they grow together, or fuse.
The soft tissues over the joint are then sewn back together. The forearm and hand are placed in a cast until the bones completely fuse together. This takes about six weeks.
Complications
What might go wrong?
As with all major surgical procedures, complications can occur. This document doesn’t provide a complete list of the possible complications, but it does highlight some of the most common problems. Some of the most common complications following thumb fusion are
- anesthesia
- infection
- nerve damage
- nonunion
Anesthesia
Problems can arise when the anesthesia given during surgery causes a reaction with other drugs the patient is taking. In rare cases, a patient may have problems with the anesthesia itself. In addition, anesthesia can affect lung function because the lungs don’t expand as well while a person is under anesthesia. Be sure to discuss the risks and your concerns with your anesthesiologist.
Infection
Any operation carries a small risk of infection. Thumb fusion surgery is no different. You will probably be given antibiotics before the operation to reduce the risk of infection. If an infection occurs you will most likely need antibiotics to cure it. You may need additional operations to drain the infection if it involves the area around the fusion.
Nerve Damage
All of the nerves and blood vessels that go to the thumb travel across, or near, the CMC joint. Since the operation is performed so close to these important structures, it is possible to injure either the nerves or the blood vessels during fusion surgery. The result may be temporary if the nerves have been stretched by retractors holding them out of the way. It is uncommon to have permanent injury to either the nerves or the blood vessels, but it is possible.
Nonunion
Sometimes the thumb bones do not fuse as planned. This is called a nonunion, or pseudarthrosis. (Pseud means false, and arthro means joint; a pseudarthrosis refers to the motion at a false joint.) If the motion from a nonunion continues to cause pain, you may need a second operation to try to get the bones to completely fuse. This usually means adding more bone graft and making sure that any metal pins that have been used are holding the bones still to allow the fusion to occur.
After Surgery
What happens after surgery?
After surgery, you will be fitted in an elbow-length cast. This gives the ends of the bones the opportunity to fuse together. Your surgeon will want to check your hand within five to seven days. Stitches will be removed in 10 to 14 days, though most of your stitches will be absorbed into your body. You may have some discomfort after surgery. You will be given pain medicine to control the discomfort.
You should keep your hand elevated above the level of your heart for several days to avoid swelling and throbbing. Keep it propped up on a stack of pillows when sleeping or sitting up.
Rehabilitation
What should I expect during my recovery period?
As mentioned, you’ll wear the cast for about six weeks to give the fusion time to heal. When the cast is removed, you may have stiffness in the joints on both sides of the fusion.
If you have pain or stiffness that doesn’t improve, you may need a physical or occupational therapist to direct your recovery program. The first few therapy treatments will focus on controlling the pain and swelling from surgery. Your therapist may use gentle massage and other hands-on treatments to ease muscle spasm and pain.
Then you’ll begin gentle range-of-motion exercise for the joints above and below the fusion. Strengthening exercises are used to give added stability around the thumb joint. You’ll learn ways to grip and support items in order to do your tasks safely and with the least amount of stress on your thumb joint. As with any surgery, you need to avoid doing too much, too quickly.
Some of the exercises you’ll do are designed get your hand and thumb working in ways that are similar to your work tasks and daily activities. Your therapist will help you find ways to do your tasks that don’t put too much stress on your thumb joint. Before your therapy sessions end, your therapist will teach you a number of ways to avoid future problems.
Your therapist’s goal is to help you keep your pain under control, improve your strength and range of motion, and regain your fine motor abilities with your hand and thumb. When your treatments are well under way, regular visits to your therapist’s office will end. Your therapist will continue to be a resource, but you will be in charge of doing your exercises as part of an ongoing home program.