A Patient’s Guide to Pain Management: Radiofrequency Ablation
Introduction
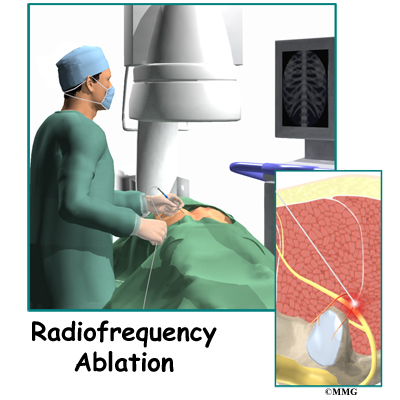
Radiofrequency ablation is a treatment where radio waves are used to create heat and destroy a part of a nerve. This technique is most commonly used to treat pain that is originating in the facet joints of the spine. The procedure is used to destroy the end of the small nerves that provide sensation to the facet joints. Once the nerve is destroyed, you should no longer feel the pain from the worn out, painful facet joints. This procedure is also sometimes called a RFA, rhizotomy, or a neurotomy.
This guide will help you understand
- What parts of the spine are involved
- What is the surgeon is trying to achieve
- What happens during the procedure
- What are the possible complications
Anatomy
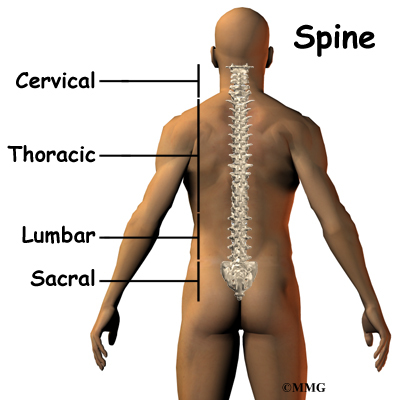
What parts make up the spine?
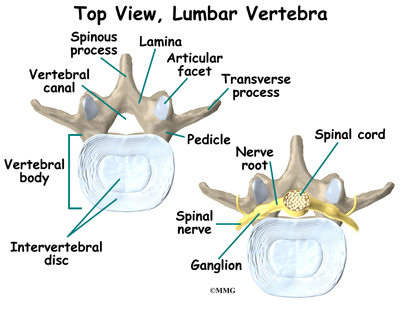
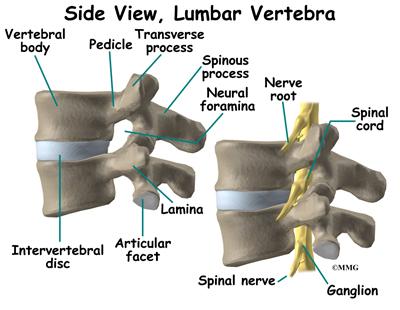
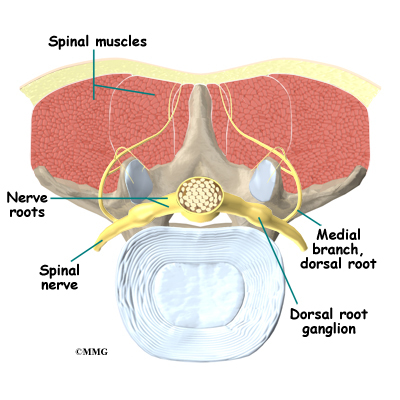
The spine is made up of 24 bones called vertebrae that stack on top of one another. Each vertebrae has a ring of bone that encases and protects the spinal cord. When the vertebra are stacked one on top of the other, these rings of bone create a hollow tube called the spinal canal. The spinal cord runs through the spinal canal from the brain to the lower spine. Between the vertebrae are intervertebral discs. The intervertebral discs cushion the spine and make it flexible. There are also two facet joints between each vertebrae of the spine. The facet joints are located on the back of the spinal column in the lumbar and thoracic spine. In the neck, or cervical spine, they are located on the each side of the vertebra.
A facet joint is a small, bony knob that extends out from the vertebral body. Where these knobs meet, they form a joint that connects the two vertebrae. The surface of the facet joints are covered by articular cartilage. Articular cartilage is a smooth, rubbery material that covers the surface of all synovial joints. It allows the bone ends to move against each other smoothly without friction. Each joint is surrounded by a joint capsule. The joint capsule is made up of the ligaments and connective tissues that help hold the joint together. The joint capsule forms a water tight sac that contains the joint fluid. The facet joints allow freedom of movement as you bend forward and back.
Like all joints, the facet joints can wear out – or degenerate. This condition is sometimes called degenerative arthritis or osteoarthritis. When this occurs in the facet joints it can cause neck and back pain. When the facet joints of the cervical spine are affected the pain can radiate into the upper back and shoulder area. When the facet joints of the lumbar spine are affected, the pain may radiate into the buttock and back of the thigh.
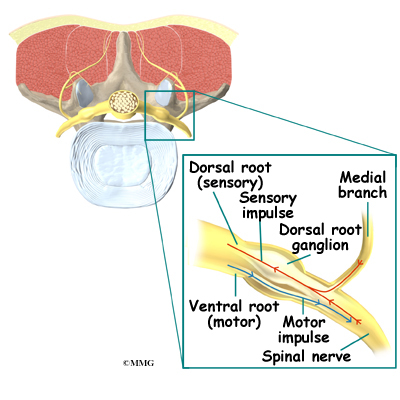
Small nerves called the medial branch nerves provide sensation to each facet joint. These nerves carry the pain signals from the facet joint to the spinal cord. The signals eventually reach the brain where you feel the sensation of pain.
Rationale
What do surgeons hope to achieve with this procedure?
There are several structures in the spine that can be a source of pain. One of the most common sources is the facet joint. As these joints degenerate and develop osteoarthritis they become painful. The pain from facet joint arthritis may come and go depending on activity.
The goal of radiofrequency ablation is to destroy the small nerves that carry the pain signal from the joint to the spinal cord. The goal is to reduce your pain, allow you to do more activity, and enable you to reduce your pain medications.
Radiofrequency ablation is usually done only after you have had a successful facet joint injection. Your doctor will perform a facet joint injection to try and determine if the facet joints are the cause of your back pain. The injection may only reduce your pain temporarily, maybe only for a few hours. Once your doctor is sure that it is the facet joint causing your pain, radiofrequency ablation is done to reduce your pain for a longer period of time. Radiofrequency ablation is not a permanent fix, but it lasts much longer than a facet joint block.
Preparation
How should I prepare for the surgery?
To prepare for the procedure your doctor may tell you to remain “NPO” for a certain amount of time before the procedure. This means that you should not eat or drink anything for the specified amount of time before your procedure. This means no water, no coffee, no tea – not anything. You may receive special instructions to take your usual medications with a small amount of water. Check with your doctor if you are unsure what to do.
You may be instructed to discontinue certain medications that affect the clotting of your blood several days before the injection. This reduces the risk of excessive bleeding during and after the injection. These medications may include the common Non-Steroidal Anti-Inflammatory Drugs (NSAIDs) such as aspirin, ibuprofen, naproxen, and many other medications that are commonly used to treat arthritis. If you are taking any type of blood thinning medication you should let your doctor know. You will most likely need to have this medication regulated or temporarily discontinued prior to the procedure. Your doctor will need to determine if it is safe to discontinue these medications in order to have the procedure.
You may need to arrange to have transportation both to and from the location where you will undergo the procedure. Wear loose fitting clothing that is easy to take off and put on. You may wish to take a shower the morning of the procedure, using a bactericidal soap to reduce chances of infection. Do not wear jewelry or any type of scented oils or lotions.
Procedure
What happens during the procedure?
When you are ready to have the procedure, you will be taken into the procedure area and an IV will be started. The IV allows the nurse or doctor to give you any medications that may be needed during the procedure. The IV is for your safety because it allows very rapid response if you have a problem during the procedure, such as an allergic reaction to any of the medications injected. If you are in pain or anxious, you may also be given medications through the IV for sedation during the procedure.
You will be awake for the procedure to help the doctor with correct placement of the electrode used for radiofrequency ablation. You will not be given a general anesthetic. The area to be treated will be cleaned and then numbed with a local anesthetic.
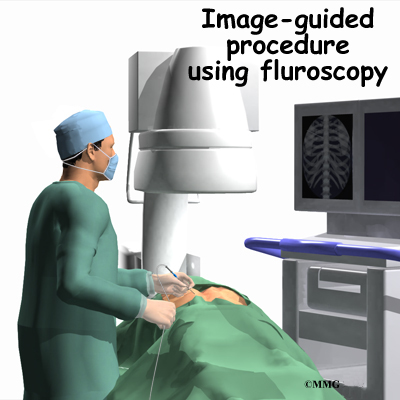
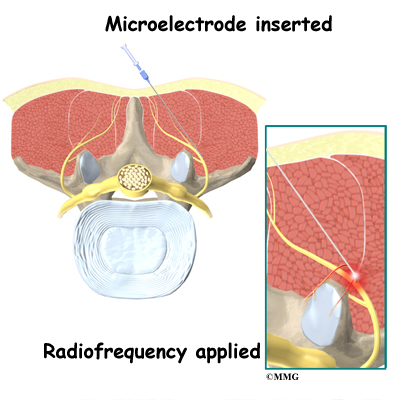
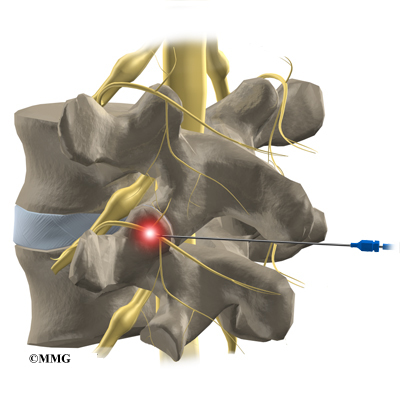
Radiofrequency ablation is done with the help of fluoroscopic guidance. The fluoroscope is an x-ray machine that allows the doctor to actually see an x-ray image while doing the procedure. This allows the doctor to watch where the needle electrode goes as it is inserted. This makes placing the electrode much safer and much more accurate. In performing radiofrequency ablation, your doctor inserts a needle electrode near the facet joint so that the tip of the needle is very near the medial branch nerve that travels to the facet joint. Once your doctor is sure that the tip of the needle is in the right place, the tip of the needle is heated to cauterize and destroy the nerve. Once the nerves carrying the sensation from the painful joints are destroyed, your pain should be reduced.
After the procedure, you will be taken to a recovery area. The nurses will monitor you to be sure you do not have an allergic reaction. You will be allowed to leave once you are stable.
Complications
What might go wrong?
There are several complications that may occur during or after the facet joint injection. Injection procedures are safe and unlikely to result in a complication, but no procedure is 100% foolproof. This document doesn’t provide a complete list of the possible complications, but it does highlight some of the most common problems. Complications are uncommon, but you should know what to watch for if they occur.
Allergic Reaction
Like most procedures where medications are injected, there is always a risk of allergic reaction. The medications that are commonly injected include lidocaine, bupivicaine, radiographic dye, and cortisone. Allergic reactions can be as simple as developing hives or a rash. They can also be life threatening and restrict breathing. Most allergic reactions will happen immediately while you are in the procedure room so that help is available immediately. Most reactions are treated and cause no permanent harm. You should alert your doctor if you have known allergies to any of these medications.
Infection
Several types of infections are possible complications of radiofrequency ablation. Any time a needle is inserted through the skin, there is a possibility of infection. Before any invasive procedure is done, the skin is cleansed with a disinfectant and the health care provider doing the procedure uses what is called sterile technique. This means that the instruments and the area where the skin is punctured remains untouched by anything that is not sterile. The doctor will also use sterile gloves.
Infections can occur just underneath the skin, in a muscle, or in the facet joint. You should watch for signs of increasing redness, swelling, pain, and fever. Almost all infections will need to be treated with antibiotics. If an abscess forms, then a surgical procedure may be necessary to drain the pus in the abscess. Antibiotics will also be necessary to treat the infection.
Nerve Damage
Many pain procedures are done close to nerves. Radiofrequency ablation is one of the safest spinal procedures because the needle electrode is usually not near the spinal nerves, but the needle electrode used to do the injection may accidentally hit a nerve while being positioned. This can cause damage to the nerve and result in increased pain. Numbness and weakness may also result. Nerves that have been punctured with a needle will usually recover and do not require any additional surgical procedures.
Neuritis
Neuritis is an inflammation of the nerve that causes pain and tenderness in the back. It may last from three to six weeks. This can occur in 10 to 15 percent of patients. Neuritis usually goes away by itself. If it does not, your doctor may suggest injecting a local anesthetic along with a steroid medication around the nerve. This may reduce the inflammation and ease your pain.
Increased Pain
Not all radiofrequency ablation procedures work as expected. Even though a test block was beneficial, some patients have no pain relief from the procedure. Even though a test block was beneficial, some patients have no pain relief from the procedure. Sometimes, the procedure can actually cause more pain. Increased pain that begins several days after the injection may be a sign of infection. You should alert your doctor if this occurs.
After Care
What should I expect after the procedure?
You will be able to go home soon after the procedure, probably within one hour. If all went as planned, you probably won’t have any restrictions on activity or diet. Immediately following the procedure, you may have some relief of pain from the numbing medication used during the procedure. You may not be able to drive or do any physical activity for 24 hours.
You may experience an increase in pain for the first several days following the procedure. Additional pain medications may be necessary to make you comfortable. If these include narcotics, you will need to watch for constipation. Drink lots of fluids and eat foods with plenty of fiber. If constipation should occur you will need to use a laxative, available over-the-counter.
You may also note some swelling and bruising where the needle was inserted. Using a cold pack may ease the discomfort.
The degree of pain relief varies from person to person. You may continue to see a decrease in your pain for up to three weeks. You may see a 50 percent or greater pain relief. Pain relief can last from 6 to 12 months, sometimes even longer. The nerves will grow back eventually and your pain will probably return. When this occurs, the procedure may be repeated.
Most doctors will arrange a followup appointment, or phone consult, within one or two weeks after the procedure to see how you are doing and what effect the procedure had on your symptoms.
And remember, radiofrequency ablation is not a cure for your pain; it is only a part of your overall pain management plan. You will still need to continue working with the other recommendations from your pain management team.