A Patient’s Guide to Lumbar Laminectomy
Introduction
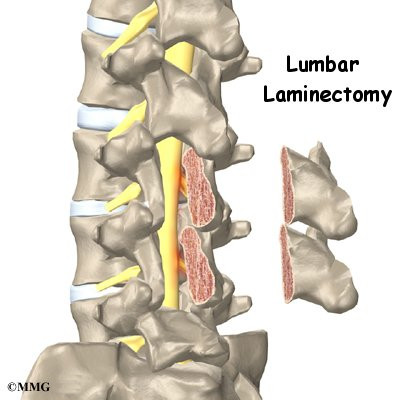
Lumbar laminectomy is a surgical procedure to relieve pressure on the spinal nerves. Degeneration, or wear and tear, in the parts of the spine may narrow the spinal canal. This puts pressure on the nerves in the canal. This condition is called spinal stenosis. A laminectomy involves removing a section of the bony covering over the back of the spinal canal. This takes pressure off the spinal nerves.
This guide will help you understand
- why the procedure becomes necessary
- what surgeons hope to achieve
- what to expect as you recover
Anatomy
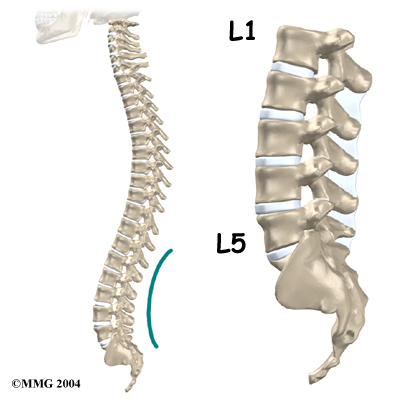
What parts of the spine are involved?
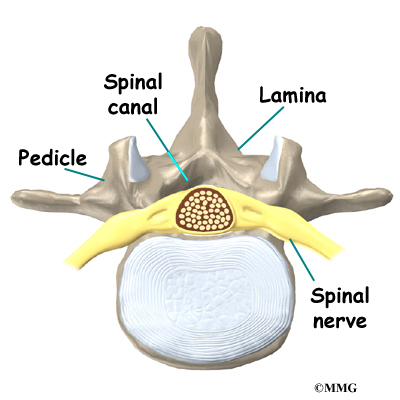
Surgeons perform lumbar laminectomy surgery through an incision in the low back. The surgery involves the pedicle and lamina bones. These bones attach to the back of the spinal column, forming a bony ring that encloses the spinal canal. Surgeons may remove bone spurs from the facet joints
along the back of the spine during the laminectomy procedure, taking pressure off the spinal nerves.
Related Document: A Patient’s Guide to Lumbar Spine Anatomy
Rationale
What do doctors hope to achieve?
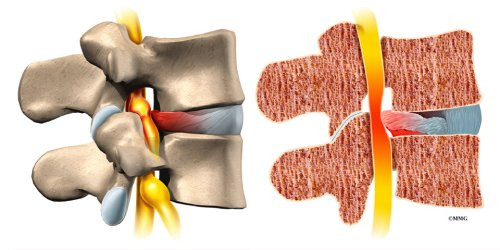
Lumbar laminectomy can alleviate the symptoms of spinal stenosis, a condition in which the spinal nerves become compressed inside the spinal canal. Wear and tear on the spine from aging and from repeated stresses and strains can cause a spinal disc to weaken.
The outer rim of the disc bulges outward, and the disc may eventually protrude or even rupture into the spinal canal, narrowing the size of the canal. As a result, the nerves inside the canal are squeezed, leading to symptoms of spinal stenosis.
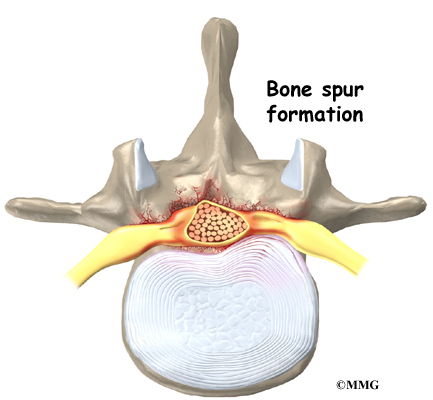
Degeneration also causes bone spurs to develop. These spurs commonly occur around the facet joints and along the edges of the vertebrae. When these spurs point into the spinal canal, they may squeeze against the spinal nerves. In a laminectomy, the surgeon removes a section of the lamina bone and any bone spurs, taking pressure off the spinal nerves. This enlarges the spinal canal so the spinal nerves have more room.
Preparations
How will I prepare for surgery?
The decision to proceed with surgery must be made jointly by you and your surgeon. You should understand as much about the procedure as possible. If you have concerns or questions, talk to your surgeon.
Once you decide on surgery, your surgeon may suggest a complete physical examination by your regular doctor. This exam helps ensure that you are in the best possible condition to undergo the operation.
On the day of your surgery, you will probably be admitted to the hospital early in the morning. You shouldn’t eat or drink anything after midnight the night before.
Surgical Procedure
What happens during the operation?
Patients are given a general anesthesia to put them to sleep during most spine surgeries. As you sleep, your breathing may be assisted with a ventilator. A ventilator is a device that controls and monitors the flow of air to the lungs.
Some surgeons have begun using spinal anesthesia in place of general anesthesia. Spinal anesthesia is injected in the low back into the space around the spinal cord. This numbs the spine and lower limbs. Patients are also given medicine to keep them sedated during the procedure.
This surgery is usually done with the patient kneeling face down in a special frame. The frame supports the patient so the abdomen is relaxed and free of pressure. This position lessens blood loss during surgery and gives the surgeon more room to work.
The surgeon makes a short incision down the middle of the low back. The skin and soft tissues are separated to expose the bones along the back of the spine. An X-ray of the low back ensures the surgeon works on the right vertebra. Some surgeons use a special surgical microscope during surgery to magnify the area they’ll be working on.
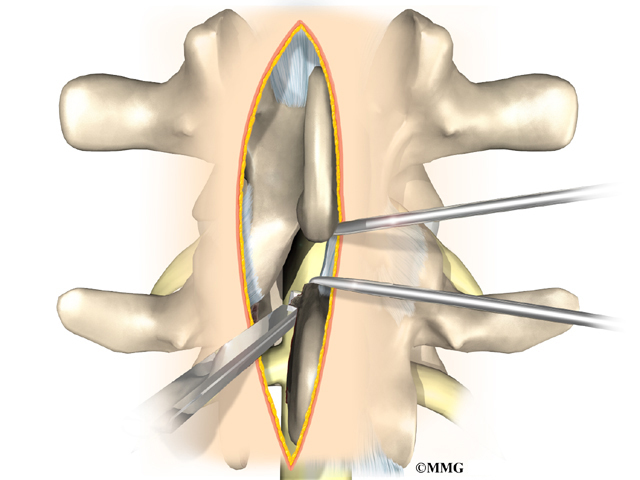
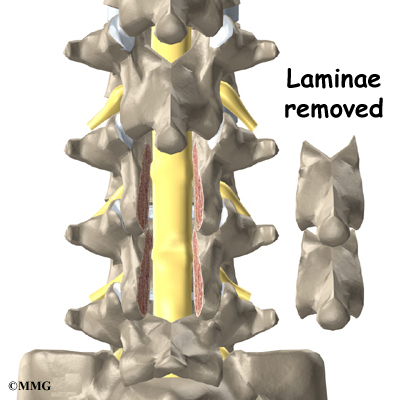
In a complete laminectomy, the spinous process (the bony projection off the back of the vertebra) and the lamina on each side are removed over the area where stenosis is occurring. To accomplish this, the surgeon cuts along the inside edge of the facet joint on each side and detaches the lamina bone completely from the pedicle bones. This opens a section in the bony ring. A small portion of the ligamentum flavum is removed. The ligamentum flavum runs all the way down the spinal canal between the lamina bones and the spinal cord. Removing a small section of this ligament exposes the nerves inside the spinal canal.
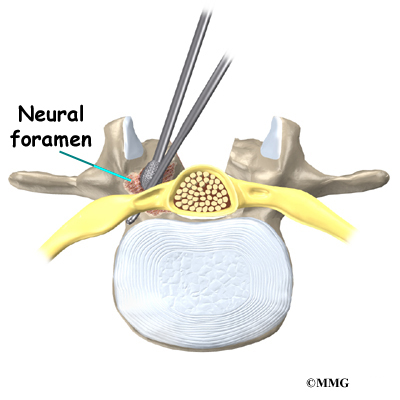
The surgeon may use small cutting instruments to carefully remove soft tissues near the spinal nerves. Then the surgeon takes out any disc fragments and scrapes off nearby bone spurs. In this way, the nerves inside the spinal canal are relieved of additional tension and pressure. The surgeon also enlarges the neural foramina, if needed. The neural foramina are the small openings between the vertebrae where the nerves travel out of the spinal canal.
The muscles and soft tissues are put back in place, and the skin is stitched together.
Complications
What might go wrong?
As with all major surgical procedures, complications can occur. Some of the most common complications following lumbar laminectomy include
- problems with anesthesia
- thrombophlebitis
- infection
- nerve damage
- segmental instability
- ongoing pain
This is not intended to be a complete list of the possible complications.
Problems with Anesthesia
Problems can arise when the anesthesia given during surgery causes a reaction with other drugs the patient is taking. In rare cases, a patient may have problems with the anesthesia itself. In addition, anesthesia can affect lung function because the lungs don’t expand as well while a person is under anesthesia. Be sure to discuss the risks and your concerns with your anesthesiologist.
Thrombophlebitis (Blood Clots)
View animation of pulmonary embolism
Thrombophlebitis, sometimes called deep venous thrombosis (DVT), can occur after any operation. It occurs when the blood in the large veins of the leg forms blood clots. This may cause the leg to swell and become warm to the touch and painful. If the blood clots in the veins break apart, they can travel to the lung, where they lodge in the capillaries and cut off the blood supply to a portion of the lung. This is called a pulmonary embolism. (Pulmonary means lung, and embolism refers to a fragment of something traveling through the vascular system.) Most surgeons take preventing DVT very seriously. There are many ways to reduce the risk of DVT, but probably the most effective is getting you moving as soon as possible. Two other commonly used preventative measures include
- pressure stockings to keep the blood in the legs moving
- medications that thin the blood and prevent blood clots from forming
Infection
Infection following spine surgery is rare but can be a very serious complication. Some infections may show up early, even before you leave the hospital. Infections on the skin’s surface usually go away with antibiotics. Deeper infections that spread into the bones and soft tissues of the spine are harder to treat. They may require additional surgery to treat the infected portion of the spine.
Nerve Damage
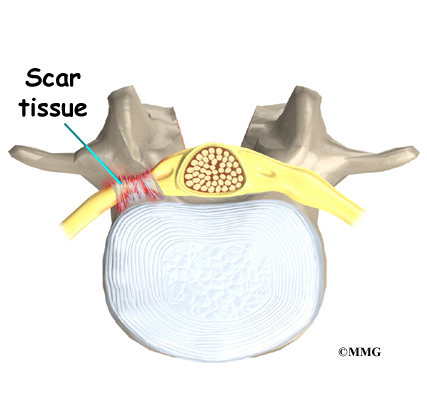
Any surgery that is done near the spinal canal can potentially cause injury to the spinal cord or spinal nerves. Injury can occur from bumping or cutting the nerve tissue with a surgical instrument, from swelling around the nerve, or from the formation of scar tissue. An injury to the spinal cord or spinal nerves can cause muscle weakness and a loss of sensation to the areas supplied by the nerve.
Segmental Instability
Laminectomy surgery can cause the spinal segment to loosen, making it unstable. Each spinal segment includes two vertebrae separated by an intervertebral disc, the nerves that leave the spinal cord at that level, and the small facet joints that link each level of the spinal column.
The facet joints on the back of the spine normally give enough stability, even when the lamina is taken off. This is why surgeons prefer not to remove the facet joints. But these joints may have to be removed if they are enlarged with arthritis or are pushing on the spinal nerves, as explained earlier. When the facet joints must be removed, additional surgery (a fusion) may be needed to fix the loose segment.
Related Document: A Patient’s Guide to Posterior Lumbar Fusion
Ongoing Pain
Many patients get nearly complete relief of symptoms from the lumbar laminectomy procedure. As with any surgery, however, you should expect some pain afterward. If the pain continues or becomes unbearable, talk to your surgeon about treatments that can help control your pain.
After Surgery
What happens after surgery?
Patients are usually able to get out of bed within a few hours after surgery. However, you will be instructed to move your back only carefully and comfortably. Patients are able to return home when their medical condition is stable.
Most patients leave the hospital the day after surgery. They are safe to drive within a week or two. People generally get back to light work by four weeks. Heavier work and sports should wait two to three months. Workers whose jobs involve strenuous manual labor may be counseled to consider different work.
Outpatient physical therapy usually starts four to six weeks after surgery.
Rehabilitation
What should I expect as I recover?
Many surgeons prescribe outpatient physical therapy within six weeks after surgery. Physical therapy after lumbar laminectomy is generally only needed for a total of four to six weeks. You should expect full recovery to take up to four months.
At first, treatments help control pain and inflammation. Ice and electrical stimulation treatments are commonly used to help with these goals. Your therapist may also use massage and other hands-on techniques to ease muscle spasm and pain.
Active treatments are added slowly. These include exercises for improving heart and lung function. Walking and swimming are ideal cardiovascular exercises after lumbar laminectomy surgery. Therapists also teach patients specific exercises to help tone and control the muscles that stabilize the low back.
Your therapist works with you on how to move and do activities. This form of treatment, called body mechanics, is used to help you develop new movement habits. This training helps you keep your back in safe positions as you go about your work and daily activities. At first, this may be as simple as helping you learn how to move safely and easily in and out of bed, how to get dressed and undressed, and how to do some of your routine activities. Then you learn how to keep your back safe while you lift and carry items and as you begin more challenging activities.
As your condition improves, the therapist tailors your program to help prepare you to go back to work. Some patients are not able to go back to a previous job that requires strenuous tasks. Your therapist may suggest changes in job tasks that enable you to go back to your previous job. Your therapist can also suggest alternate forms of work. You’ll learn to do your tasks in ways that keep your back safe and free of extra strain.
Before your therapy sessions end, your therapist will teach you a number of ways to avoid future problems.