A Patient’s Guide to Kyphoplasty
Introduction
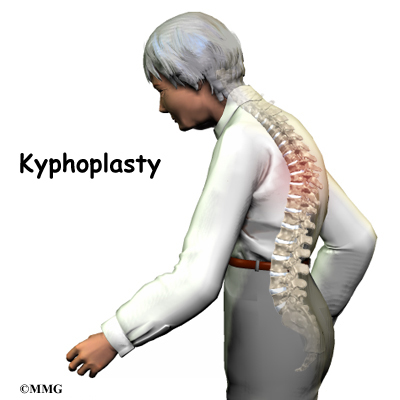
Patients with osteoporosis are prone to compression fractures in the spine bones, or vertebrae. The bone cracks under pressure, causing it to collapse in height. More than 700,000 such fractures occur every year in the United States.
The fracture angles the spine forward and produces a hunchbacked appearance, called kyphosis. Patients with this condition are subject to debilitating pain, disturbed sleep, decreased lung and intestinal function, and difficulty completing routine activities.
Kyphoplasty restores the size and strength of the fractured vertebra. This realigns the spine and reduces pain. Nearly 95 percent of patients get immediate relief of pain with this procedure.
This guide will help you understand
- why the procedure becomes necessary
- what surgeons hope to achieve with kyphoplasty
- what to expect during recovery
Anatomy
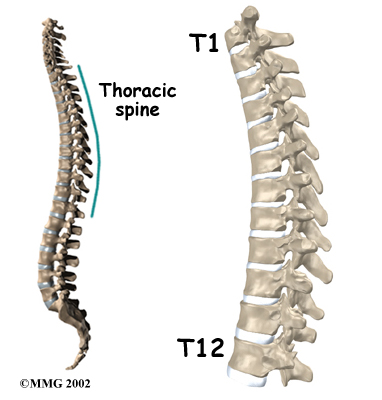
What parts of the spine are involved?
The main section of each spine vertebra is a large, round structure called a vertebral body. Compression fractures cause the front portion of this round bone to collapse in height. Because the back section of the bone stays intact, the damaged vertebral body becomes wedge-shaped.
It is this wedge shape that angles the spine forward into kyphosis. The vertebral body is the main structure treated in the kyphoplasty procedure.
Related Document: A Patient’s Guide to Thoracic Spine Anatomy
Rationale
What do surgeons hope to achieve with this procedure?
In the past, surgeons used standard open surgical procedures to fix compression fractures from osteoporosis. Open procedures require larger incisions to give the surgeon more room to operate. The results of open surgery for this condition have generally been poor, mainly because operating on bones that are weak and soft from osteoporosis is difficult. In addition, some aging adults with fractures may not be physically able to tolerate such a surgery.
Kyphoplasty gives surgeons a way to fix the broken bone without the problems associated with open surgery. Unlike open surgery, which involves an incision and the use of larger instruments, kyphoplasty is a minimally invasive procedure. It requires a small opening in the skin and small instruments. This lessens the chance of bleeding, infection, and injury to muscles and soft tissues.
The goal of kyphoplasty is to return the fractured vertebra as close as possible to its normal height. This is done by inflating a balloon inside the fractured bone to restore the vertebral body to its normal size. Special cement is then injected into the bone, fixing it in place. The cement strengthens the broken vertebra and stiffens it in its original height and position. This reduces pain and spine deformity (kyphosis), enabling patients to get back to normal activities.
Related Document: A Patient’s Guide to Spinal Compression Fractures
Preparations
How will I prepare for the procedure?
The decision to proceed with kyphoplasty must be made jointly by you and your surgeon. You should understand as much about the procedure as possible. If you have concerns or questions, talk to your surgeon.
Kyphoplasty is normally done on an outpatient basis, meaning patients go home the same day as the surgery. You shouldn’t eat or drink anything after midnight the night before.
Surgical Procedure
What happens during the procedure?
The patient lies on his or her stomach. To begin, the surgeon cleans the skin on the back with an antiseptic. Then the skin over the problem area is numbed using an anesthetic. Patients may also receive general anesthesia to put them to sleep during the procedure.
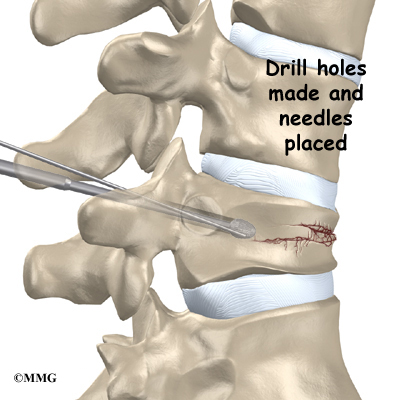
Two small openings are made in the skin on each side of the spinal column. Long needles are inserted through the openings. The needles are passed completely through the back of the spinal column into the fractured vertebral body. These needles serve as guides while the surgeon drills two holes into the vertebral body. The surgeon uses a fluoroscope to make sure the needles and drill holes are placed in the right spot. A fluoroscope is a special X-ray television that allows the surgeon to see your spine on a screen.
The device works like a video, though the images are in the form of an X-ray. Metal objects show up clearly on X-rays. The needle is easy for the surgeon to see on the fluoroscope screen. This helps the surgeon know the needle goes into the correct spot.
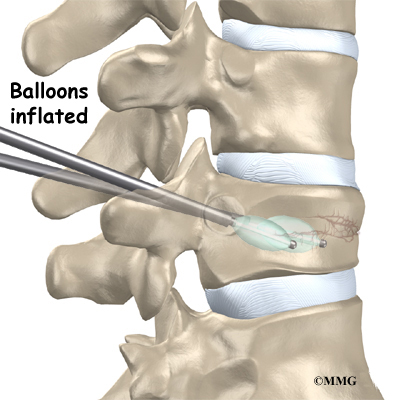
A hollow tube with a deflated balloon on the end is then slid through each drill hole. The balloons are inflated with air. This restores the height of the vertebral body and corrects the kyphosis deformity.
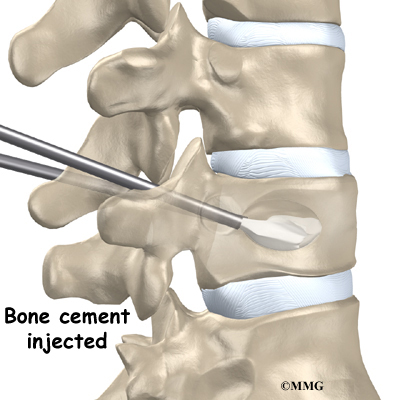
Next, the surgeon removes the balloon and injects bone cement into the hollow space formed by the balloon. A chemical reaction in the cement causes it to harden in about 15 minutes.
This fixes the bone in its corrected height and position. Bandages are then applied over the small incisions.
Complications
What might go wrong?
Serious complications from kyphoplasty are rare, involving less than five percent of cases. As with other procedures, however, complications can occur. Some of the most common complications of kyphoplasty include
- problems with anesthesia
- thrombophlebitis
- infection
- cement leakage
- ongoing pain
This is not intended to be a complete list of the possible complications.
Problems with Anesthesia
Problems can arise when the anesthesia given during surgery causes a reaction with other drugs the patient is taking. In rare cases, a patient may have problems with the anesthesia itself. In addition, anesthesia can affect lung function because the lungs don’t expand as well while a person is under anesthesia. Be sure to discuss the risks and your concerns with your anesthesiologist.
Thrombophlebitis (Blood Clots)
View animation of pulmonary embolism
Thrombophlebitis, sometimes called deep venous thrombosis (DVT), can occur after any operation. It occurs when the blood in the large veins of the leg forms blood clots. This may cause the leg to swell and become warm to the touch and painful. If the blood clots in the veins break apart, they can travel to the lung, where they lodge in the capillaries and cut off the blood supply to a portion of the lung. This is called a pulmonary embolism. (Pulmonary means lung, and embolism refers to a fragment of something traveling through the vascular system.) Most surgeons take preventing DVT very seriously. There are many ways to reduce the risk of DVT, but probably the most effective is getting you moving as soon as possible. Two other commonly used preventative measures include
- pressure stockings to keep the blood in the legs moving
- medications that thin the blood and prevent blood clots from forming
Infection
Infection following spine procedures is rare but can be a very serious complication. Some infections may show up early, within the first few days after the procedure. Infections on the skin’s surface usually go away with antibiotics. Deeper infections that spread into the bones and soft tissues of the spine are harder to treat. They may require surgery to treat the infected portion of the spine.
Cement Leakage
The cement used in kyphoplasty is squeezed into the fractured vertebra in liquid form. Because it is injected at low pressure, cement leakage during kyphoplasty is rare. If some of the cement happens to leak out of the vertebra, it usually doesn’t cause any problems. Only rarely does a cement leak cause pressure on the spinal cord or nearby nerves. In these cases, surgery may be required to remove the pressure.
Ongoing Pain
Many patients get nearly complete relief of symptoms from kyphoplasty. As with any procedure, however, you should expect some pain afterward. If the pain continues or becomes unbearable, talk to your surgeon about treatments that can help control your pain.
After Surgery
What happens after surgery?
Patients are monitored in the recovery room for two to three hours after the procedure before going home. You are instructed to move your back only carefully and comfortably. Some patients who are feeling extra pain or other problems after kyphoplasty may need to stay in the hospital overnight.
Patients rarely need to wear a brace after kyphoplasty, since bone cement immediately improves the strength and stiffness in the fractured vertebra.
Rehabilitation
What should I expect as I recover?
The cement used to fix the broken vertebra hardens quickly, within about 15 minutes. As a result, people often find it easier to do daily activities within one week. Pain also decreases rapidly, and most people require less pain medication within two weeks. Despite these improvements, most orthopedists consider that it takes about three months for the bone to heal after kyphoplasty.
Patients are encouraged to walk and do moderate activity as they recover. However, they should avoid strenuous exertion until their surgeon approves resuming normal levels of activity.
When the fracture was from osteoporosis, the doctor will suggest ways to prevent future problems. Patients may be prescribed medications and supplements (calcium and vitamin D) to maximize bone health. Lifestyle changes, such as quitting smoking and taking up exercising, may also be discussed.
Related Document: A Patient’s Guide to Osteoporosis
Patients who continue to have problems with posture and pain or who have lost muscle tone and strength may need the help of a physical therapist. These patients typically need to attend therapy sessions for four to six weeks.
The goal of therapy is to safely advance strength and function.
The therapist may use treatments such as heat or ice, electrical stimulation, and massage to help calm pain. Gentle exercise is used to improve strength of the spine and limbs. Patients begin learning how to move safely using healthy postures to reduce strain on the healing back. Exercises for the heart and lungs improve stamina and help with pain control.
As the therapy sessions come to an end, the therapist helps patients get back to the activities they enjoy. Ideally, patients are able to resume normal activities. They may need guidance on which activities are safe or how to change the way they go about their activities.
When treatment is well under way, regular visits to the therapist’s office will end. The therapist will continue to be a resource. But patients are in charge of doing their exercises as part of an ongoing home program.